Estimating the Spillover Impact of IRA Part B Negotiation
Summary
A survey finds that reimbursement contracts outside Medicare FFS still reflect Medicare metrics, raising questions about broader Part B negotiation effects.As the new Trump administration is poised to take over Medicare drug price negotiations, stakeholders are closely monitoring how the negotiation process may evolve in the next four years. This spring, the Centers for Medicare & Medicaid Services (CMS) plans to release draft guidance for the third cycle of the Medicare Drug Price Negotiation Program, which for the first time will include physician-administered drugs covered under Part B. Given the complex nature of various government pricing definitions, the impact of Medicare negotiation for Part B drugs may have direct spillover effects in the commercial market.
Background
Under statutory language included in Sec. 1847A, Congress directs CMS to reimburse physicians for the cost of Part B drugs in Medicare fee-for-service (FFS) at the manufacturer’s average sales prices (ASP) plus a 6% add-on payment to cover a range of fixed overhead costs. Such costs include expenses associated with proper storage, shipping, handling, inventory management, IT infrastructure, patient bad debt, and compliance with drug compounding and preparation requirements, to name a few. Under the Inflation Reduction Act (IRA), reimbursement for negotiated drugs will get reduced to the negotiated maximum fair price (MFP) +6%, effectively cutting provider payment for these products, despite the potential for practice overhead costs for those drugs to remain unchanged.
The IRA impact on providers could also extend outside of Medicare FFS. Price concessions associated with the MFP are not excluded from government price reporting, so both Best Price and ASP for negotiated drugs are also likely to steadily decline over time. This in turn would lower reimbursement in Medicare Advantage (MA) and private insurance plans for providers whose contracts are tied to ASP as a pricing metric. A recent Avalere analysis finds that physicians could lose at least $25 billion in add-on payments for the 10 Part B drugs expected to be negotiated first.
To better understand the impact of potential IRA Part B negotiations in the commercial market, Avalere surveyed MA and commercial payer organizations on how prevalent ASP-based contracts are and how focused payers may be on implementing changes to their reimbursement rates.
Survey Findings
Avalere’s survey included 50 representatives from national and regional payer organizations, representing over 250 million lives in the commercial market and MA. There were two key findings:
1. ASP remains a key reimbursement metric outside of Medicare FFS. The survey revealed that a significant portion of payers continue to use reimbursement methodologies that mirror Medicare, with “ASP+6%” and the “Medicare Allowable” amount having the highest use among payers (Figure 1). The degree of IRA impact on physicians outside of Medicare FFS could be impacted based on how many contracts are tied to reimbursement methodologies impacted by the MFPs.
Figure 1. Percent of Payer Respondents Using Certain Provider Reimbursement Methodologies
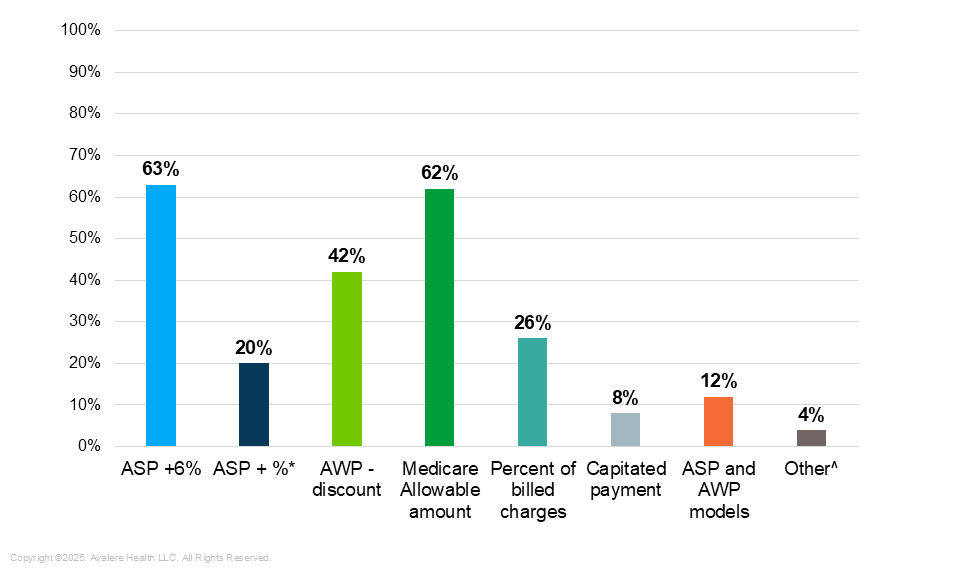
* One respondent indicated that the percentage add-on for their ASP + % reimbursement methodology in provider contracts was proprietary.
^Two respondents indicated their organization utilizes “value-based” reimbursement methodologies.
Note: Subtotals do not equal 100% since respondents may use multiple reimbursement metrics across contracts.
AWP: Average Wholesale Price
2. Other contract terms, such as contract length, can impact the magnitude and timing of IRA impacts. Over 80% of respondents across both MA and commercial markets reported contract duration of two or more years with providers. About 20% of respondents indicated that their organization is contemplating reimbursement methodology changes over time due to certain policies and market trends.
What’s Next?
Changes in payment for Part B drugs selected for negotiation could lead to changes in prescriber behavior, impact consolidation incentives, or prompt site of care shifts. Policymakers should consider the potential spillover impact of Medicare Part B negotiations and its potential implications for patient access to treatments.
To learn more about the impact of Medicare drug price negotiation, as well as other IRA drug pricing provisions, connect with an Avalere expert today.






