White Paper: The Role of PBMs in the US Healthcare System
Summary
A new white paper describes the role of PBMs in the US healthcare system using evidence published in the literature to inform future discussions.Pharmacy benefit managers (PBMs) administer prescription drug benefits for over 275 million Americans, supporting a variety of plan sponsors including commercial health plans, self-insured employers, union plans, Medicare Part D, and managed Medicaid plans. To assess the evolving role of PBMs within the US healthcare landscape, Avalere Health conducted a targeted literature review. Our search strategy was designed to capture relevant publications focusing on (1) PBM history and evolution context, (2) PBM impact on drug costs, access and outcomes, and (3) emerging trends and future directions for PBMs. We discuss our findings in a paper that aims to describe the role of PBMs in the US healthcare system using evidence to inform the current policy debate.
PBMs in the US Healthcare System
In contract negotiations, plan sponsors and PBMs negotiate the services provided, ranging from administrative functions like claims processing to clinical functions like safety and clinical programs.
Figure 1. Range of Key Services PBMs Provide to their Clients

PBMs can improve member health outcomes through clinical programs. Evidence shows that member and provider outreach programs can increase medication adherence by up to 16% for members with chronic conditions. Additionally, drug therapy management programs can help members better manage their chronic conditions and coordinate their care; a study published in the American Journal of Managed Care found a 10.4% reduction in inpatient visits and 2.6% reduction in emergency department utilization.
PBMs can also generate cost savings on behalf of plan sponsors through negotiations with life science companies and network pharmacies. According to a 2019 report from the US Government Accountability Office, PBMs worked with plan sponsors to manage drug benefits and negotiate rebates to offset Part D spending by 20%. A research paper from the National Bureau of Economic Research estimated that PBMs generate at least a net of $145 billion annual savings.
Over the past few years, PBMs have faced increased scrutiny from policymakers, regulators, and the public. In 2022, the Federal Trade Commission launched an investigation into PBM business practices. Congress has also been exploring PBM reform, with at least four pending bills in the Senate and 16 pending bills in the House. At the state level, 35 states have enacted at least one bill covering non-PBM affiliated pharmacy reimbursements, patient cost sharing, rebate pass through, spread pricing, PBM reporting, white bagging, and delinking since 2023.
Figure 2. State Bills to Regulate PBM Activities in Select Topics, 2023–2025
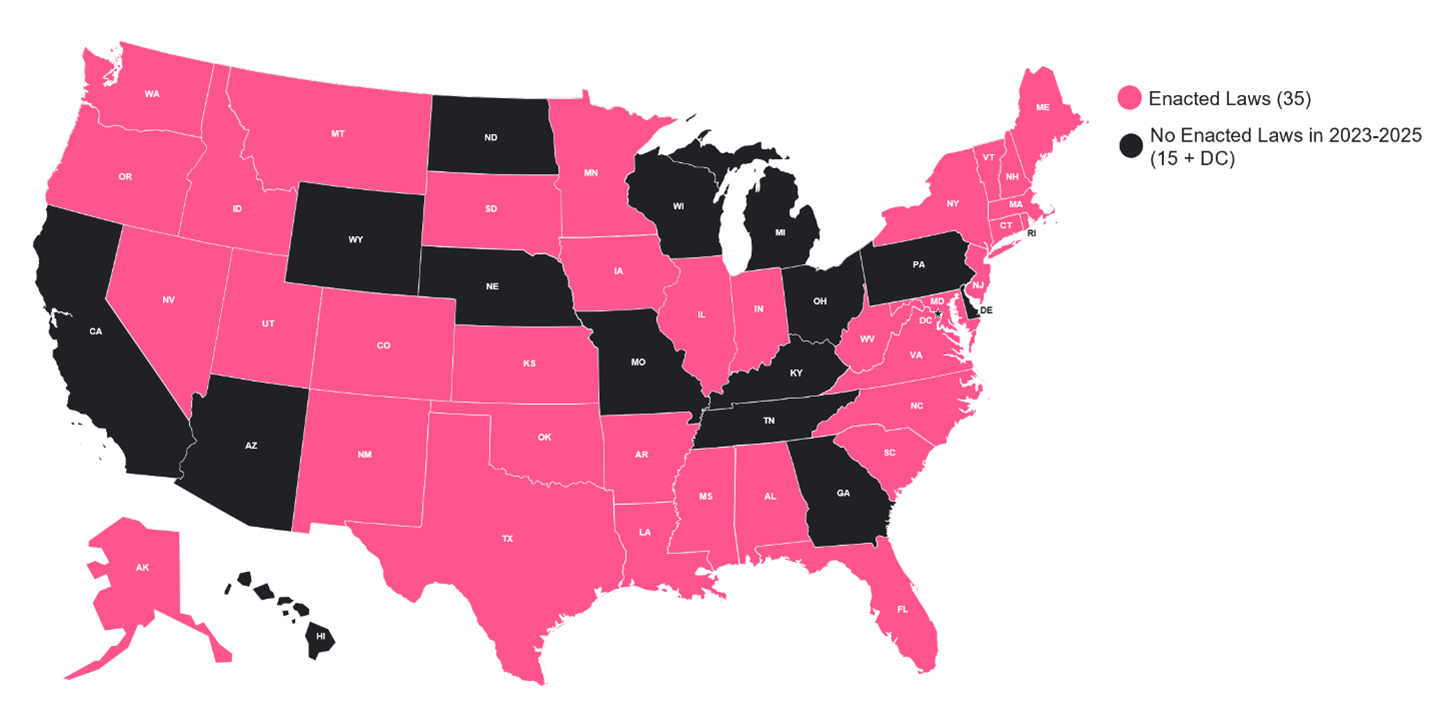
This heightened attention is largely due to concerns regarding some PBM practices and the impact on prescription drug prices and access. Critics argue that vertical integration with health plans and other entities, as well as consolidation within PBMs, have adversely affected the affordability and accessibility of medications.
The healthcare ecosystem is inherently complex, with multiple stakeholders involved, creating an environment where the nuances of relationships and impacts are not easily untangled. For a constructive debate around legitimate concerns of efficiency and affordability in the pharmaceutical market, stakeholders should take a wholistic approach that balances the calls for increased transparency and timely access with the understanding of how PBMs can serve as tools for efficiency—driving competition, reducing costs, and improving adherence.
Funding for this research was provided by Evernorth Health Services. Avalere Health retained full editorial control.



